Program curriculum is modeled by the requirements set by the ACGME. The curriculum is designed to prepare residents to enter their advanced residency training with a comprehensive skillset, including utilization of technology and engagement in high quality multidisciplinary techniques.
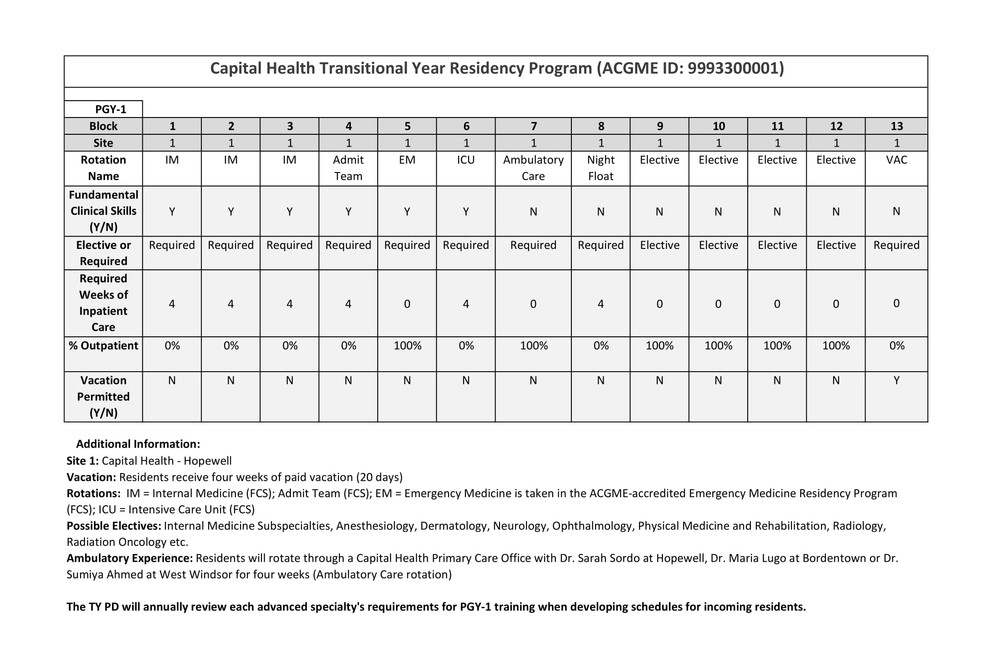
The Transitional Year Residency curriculum consists of 13 four-week blocks. During the one-year program, residents will meet the following requirements:
- 24 weeks of fundamental clinical skills in the primary specialties of inpatient internal medicine, emergency medicine and critical care medicine.
- Ambulatory Care four-week block to meet requirement of 140 hours uninterrupted by inpatient activities.
- 16 weeks of various general elective rotations, including four weeks of surgical elective rotations
Internal Medicine
The inpatient Internal Medicine rotations represent the largest quantity (12 weeks) of assigned time in a resident's schedule, and therefore present some of the most significant opportunities for gaining knowledge and experience. Transitional Year residents are integrated into Internal Medicine and Family Medicine Resident teams on Telemetry floors. Residents are the primary provider of care to their patients, under the supervision of Internal Medicine Faculty physicians. Residents have regular interactions and teaching with sub-specialist physicians.
Admit Team
The Admit Team rotation (4 weeks) is designed to achieve several educational and operational goals. Transitional Year residents’ role on the Admit Team is to perform admissions during regular work hours with the Hospitalist Admitter. This allows members of the Admit Team to focus exclusively on the history and physical, including assessment and plan, admission orders, and communication with attending physicians and consultants, without the need to be responsible for rounding, covering pages, and progress note writing. Conversely, the Admit Team offloads the regular inpatient teams from doing as many admissions during regular working hours, allowing them to focus more on their work of rounding, notes, and ongoing care of medical inpatients.
Critical Care
The critical care rotation (4 weeks) is designed to expose residents to the most seriously ill patients in the hospital, with a wide variety of cardiac, pulmonary, infectious and other multisystem diseases. This experience requires particular attention to cultivating skills in patient care and medical knowledge, but the other competencies are highlighted during this rotation as well. Residents may view the critical care rotation as a time when they may bring all their skills to bear simultaneously in the care of the sickest patients in the hospital under the supervision of board certified intensivists. Intensivists lead multidisciplinary teaching rounds daily and are available 24 hours a day, seven days a week to supervise residents directly or indirectly by telephone. Teaching consultants are also involved in critical care cases to supervise the portions of the case relevant to their specialty. Transitional Year residents work together with residents from Internal Medicine, Emergency Medicine and Family Medicine programs.
Emergency Medicine
During the Emergency Medicine rotation (4 weeks), residents will work under the supervision of Emergency Medicine attending physicians along with residents in our ACGME-accredited Emergency Medicine Program to triage, interview, diagnose and manage unselected patients who present to the Emergency Department. Residents will participate in didactic sessions with Emergency Medicine Residents during this rotation. This rotation will improve differential diagnosis insight and skills in diagnosis, clinical decision making and management of urgent/emergent situations.
Ambulatory Care
Residents receive their ambulatory care experience at a Capital Health Primary Care office with Dr. Sarah Sordo, Dr. Maria Lugo or Dr. Sumiya Ahmed. This experience (4 weeks) is designed to expose residents to the breadth and depth of medical problems seen in the office setting allowing residents to be involved in the full range of activities seen in the outpatient setting, including the coordination of care and communication between specialists, hospital-based, and primary-care physicians.
Night Float
The primary educational objective of the night float rotation (4 weeks) is to provide residents with an important opportunity to triage, assess and manage patients, develop independent thought and exercise of judgment in patient care. Transitional Year residents work together with Family Medicine senior residents under supervision of nocturnist hospitalists. They perform admissions and cover acute issues on telemetry floor at night. Emergency Department physicians are available for assistance as well as consultants in all specialties on call.
Electives
Residents have 16 weeks of elective time that allows them to personalize the program to support their endeavors into the specialty of their choice. Possible electives include internal medicine subspecialties, anesthesiology, dermatology, ophthalmology, pain management, physical medicine and rehabilitation, radiology, radiation oncology, wound care and others. These experiences are designed to provide residents with advancement in their patient care, medical knowledge, practice-based learning and improvement, interpersonal and communication skills, professionalism, and systems-based practice competencies.
Residents are also granted four weeks of approved “away” elective time. To get “away” elective approval, residents must arrange with an attending preceptor at the visiting institution and notify the program coordinator, chief resident, and elective attending preceptor of such arrangements at least six weeks in advance of rotation start date. Residents will complete the ‘Request for Outside Elective Form’ electronically and submit to the program.